6130 N La Cholla Blvd, Suite 111 Tucson, AZ 85741
Looking for trusted hyperbaric oxygen therapy in Tucson? You’ve come to the right place. Hyperbaric Oxygen Therapy, or HBOT, is a medical treatment that enhances the body’s natural healing process by delivering pure oxygen in a pressurized chamber. By increasing oxygen levels in the blood, HBOT helps promote faster wound healing, reduce inflammation, and support recovery. Whether recovering from an injury or managing a chronic condition, HBOT could be the solution a patient needs.
Approved indications treated in an outpatient setting include:
Hyperbaric Oxygen Therapy is a medical treatment in which a patient breathes 100% pure oxygen inside a pressurized chamber. The pressure inside the chamber is typically 1.5 to 3 times higher than normal atmospheric pressure. Under these conditions, your lungs can take in significantly more oxygen than they can at normal pressure. This oxygen is then dissolved into your blood plasma and carried throughout your body—even into areas with reduced or blocked blood flow. HBOT has been approved by the Undersea & Hyperbaric Medical Society (UHMS) and the Centers for Medicare & Medicaid Services (CMS) for specific conditions, including certain types of chronic, non-healing wounds.
You may qualify for Hyperbaric Oxygen Therapy (HBOT) if:
1. You Have a Wound or Condition Approved for HBOT
The Undersea & Hyperbaric Medical Society (UHMS) and Centers for Medicare & Medicaid Services (CMS) recognize HBOT for specific conditions, including:
2. Your Wound Has Not Healed with Standard Care
Most insurance plans require that the wound:
3. You Meet Safety Requirements
Before starting HBOT, your provider will:
4. You Complete a Wound Care Center Evaluation
At your first visit, the team will:
Here’s a step-by-step overview of what typically happens during a Hyperbaric Oxygen Therapy (HBOT) treatment:
1. Preparation Before Treatment
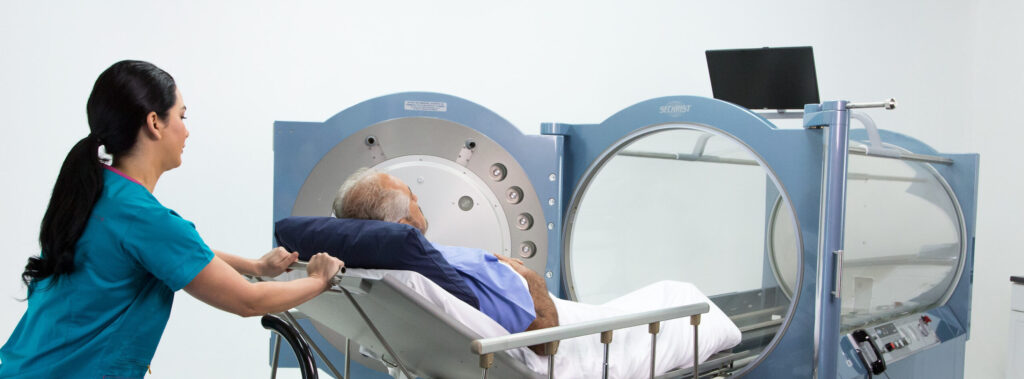
2. Entering the Monoplace Chamber
3. Pressurization (“Descent”)
4. Breathing 100% Oxygen
5. Depressurization (“Ascent”)
6. After Treatment